In Singapore, diabetes is often referred to as a “national disease”. With our fast-paced lifestyle, food culture, and ageing population, more Singaporeans are living longer, but also managing multiple chronic conditions at once. One issue that is far less talked about, yet deeply impactful, is the link between diabetes and incontinence.
For many people, frequent urination, urgency, or bladder leaks are dismissed as “just part of ageing”. Others feel too embarrassed to bring it up, even with family or healthcare professionals. But urinary and bowel incontinence can be a warning sign or a complication of diabetes, and it is something that can be managed with the right knowledge, care, and support.
At TrueHugz, we believe education is the first step toward dignity and confidence. This article explains how diabetes and incontinence are connected, who is most at risk in Singapore, and how individuals and caregivers can prevent, manage, and live well despite these challenges.
According to Singapore health data, more than 1 in 3 adults aged 60 and above lives with diabetes, and many younger adults are being diagnosed earlier than before. Type 2 diabetes is the most common form, often linked to lifestyle factors such as diet, physical inactivity, stress, and genetics.
What is less commonly discussed is that diabetes affects more than just blood sugar levels. Over time, poorly controlled diabetes can damage nerves, muscles, and blood vessels including those that control the bladder and bowels. This is where incontinence comes in.
Incontinence refers to the loss of bladder or bowel control, ranging from mild leaks to complete inability to hold urine or stool. It is not a disease on its own, but a symptom of underlying issues and diabetes is a major contributor.
Common types of incontinence linked to diabetes include:
• Urge incontinence (sudden, strong need to urinate)
• Nocturnal incontinence (frequent urination, with involuntary leakage)
• Overflow incontinence (bladder not emptying fully)
• Functional incontinence (unable to reach the toilet in time due to mobility issues)
• Bowel incontinence (less common, but possible with nerve damage)
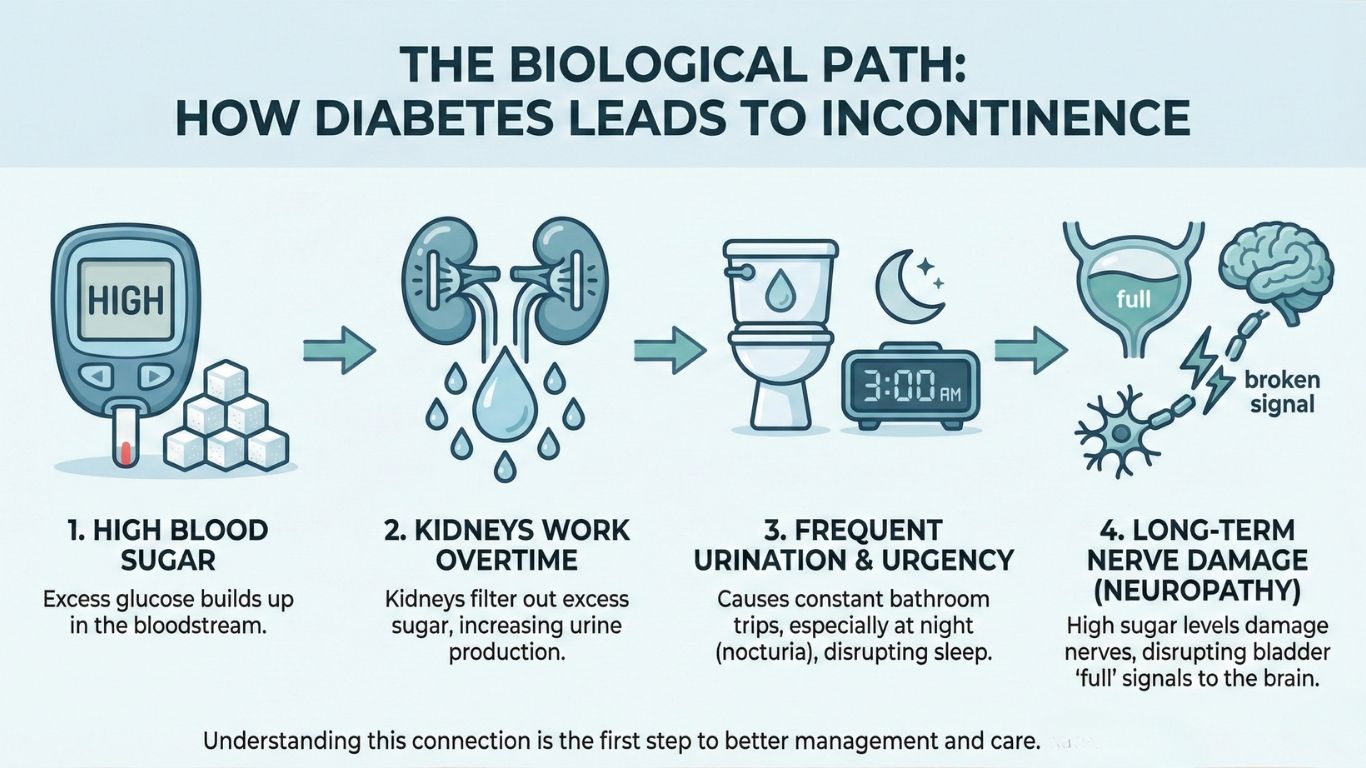
1. High Blood Sugar Causes Excessive Urination
When blood sugar levels are consistently high, the kidneys work overtime to remove excess glucose from the body. This leads to increased urine production, causing:
• Frequent trips to the toilet
• Sudden urgency
• Night-time urination that disrupts sleep
Over time, this constant pressure weakens bladder control, especially in older adults.
2. Diabetic Neuropathy Affects Bladder Nerves
One of the most serious long-term complications of diabetes is nerve damage (neuropathy).
When nerves controlling the bladder are damaged:
• The bladder may not signal when it is full
• The bladder may not empty completely
• Leakage or overflow can occur without warning
This condition, sometimes called diabetic bladder dysfunction, is more common than many realise yet often undiagnosed.
3. Weakened Pelvic Floor Muscles
Diabetes can affect muscle strength and coordination, including the pelvic floor muscles that support bladder and bowel control. This is especially relevant for:
• Older adults
• Women after childbirth or menopause
• Individuals with limited mobility or long-term illness
Weak pelvic muscles increase the risk of leaks during movement, coughing, or transfers.
4. Higher Risk of Urinary Tract Infections (UTIs)
People with diabetes are more prone to UTIs due to:
• Sugar in the urine encouraging bacterial growth
• Incomplete bladder emptying
• Reduced immune response
Repeated UTIs can worsen urgency, pain, and incontinence symptoms.
5. Bowel Issues and Diarrhoea
In some cases, long-term diabetes affects the nerves of the digestive system, leading to:
• Chronic diarrhoea
• Loss of bowel control
• Constipation followed by leakage
These symptoms are often distressing and misunderstood, but they are medical complications, not personal failures.
In the Singapore context, the following groups are particularly at risk of developing incontinence linked to diabetes, or of managing both conditions at the same time:
• Seniors aged 60 and above
• Individuals with long-standing or poorly controlled diabetes
• Care-dependent adults in home or nursing care
• People with mobility limitations or disabilities
• Patients managing multiple health needs at once
Because many Singaporean families rely on family caregivers or domestic helpers, incontinence management often becomes a shared responsibility, making education even more important.
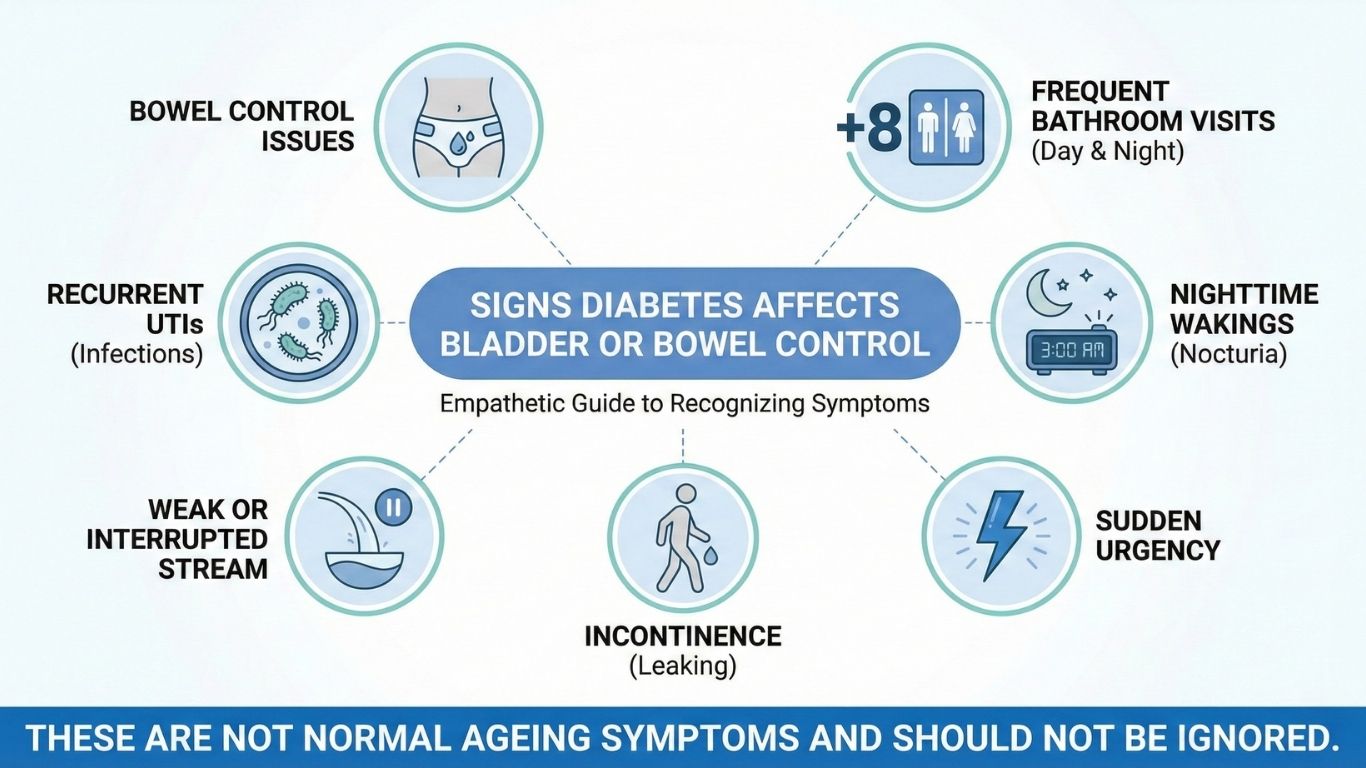
If you or a loved one has diabetes, watch out for these signs:
• Urinating more than 8 times a day
• Waking multiple times at night to urinate
• Sudden urgency with little warning
• Leaks during movement or transfers
• Difficulty starting or finishing urination
• Unexplained bowel accidents
These are not normal ageing symptoms and should not be ignored.
1. Keep Blood Sugar Levels Well Controlled
The most important step is good diabetes management:
• Follow prescribed medication or insulin schedules
• Monitor blood glucose regularly
• Attend routine medical check-ups
Stable blood sugar reduces stress on the bladder and nerves.
2. Train the Bladder
Bladder training techniques can help improve control:
• Scheduled toilet visits
• Gradually increasing time between urination
• Avoiding “just in case” trips that weaken bladder signals
This should be done gently and consistently.
3. Strengthen Pelvic Floor Muscles
Pelvic floor exercises can benefit both men and women:
• Improve bladder support
• Reduce leaks
• Enhance confidence during daily activities
A physiotherapist or continence nurse can guide proper technique.
4. Manage Fluid Intake Smartly
Avoid cutting fluids excessively, dehydration can worsen UTIs.
Instead:
• Reduce caffeine and sweetened drinks
• Space fluids evenly throughout the day
• Limit fluids 2–3 hours before bedtime to reduce nocturia
5. Address Mobility and Accessibility
Incontinence is often worsened by delays reaching the toilet.
Helpful adjustments include:
• Clear pathways at home
• Bedside commodes or urinals
• Easy-to-remove clothing
• Pull-up or tab-style incontinence products suited to mobility level (TrueHugz)
6. Use the Right Incontinence Products
High-quality incontinence products play a crucial role in dignity and skin health.
When choosing products:
• Match absorbency to urine output
• Ensure breathability to protect skin
• Choose designs that fit lifestyle and mobility needs
TrueHugz products are designed with comfort, discretion, and Singapore’s humid climate in mind, supporting both users and caregivers.

At TrueHugz, we believe that living with diabetes or incontinence should never mean living with embarrassment or isolation. Our mission is to provide credible education, thoughtful care solutions, and a supportive community for users and caregivers across Singapore.
Because managing health is not just about treatment, it’s about quality of life.
Reference
1. HealthHub Singapore
2. National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
Diabetes, Sexual and Bladder Problems
3. Mayo Clinic
Diabetic Neuropathy – Symptoms and Causes
4. Healthline
Please sign in first.
Sign in
Create a free account to save loved items.
Sign in